Two Diseases, One Map: What The Geography Of ALS And MS Might Tell Us About Your Immune System

If You Live With Autoimmune Fatigue, This Research Is For You
If you live with an autoimmune condition, you know that fatigue is not just being tired. It is the kind of bone-deep exhaustion that does not go away with rest, and your body seems to be fighting itself from the inside out.
That internal conflict is driven, in large part, by systemic inflammation. A new study published in Scientific Reports (Nature) suggests that this inflammation may connect two serious neurological diseases in a way researchers have never fully recognized — with implications that reach well beyond either disease alone.
A Surprising Discovery In The Data
Researchers at New York University analyzed death certificate data for more than 53,000 Americans who died from either ALS (amyotrophic lateral sclerosis, also known as Lou Gehrig’s disease) or MS (multiple sclerosis) between 2018 and 2022.
What they found was striking: states where MS is more common also tend to have higher rates of ALS. This geographic overlap held up even after the researchers controlled for race, income, access to neurologists, gender, and latitude. The same pattern was confirmed using World Health Organization data from dozens of countries.
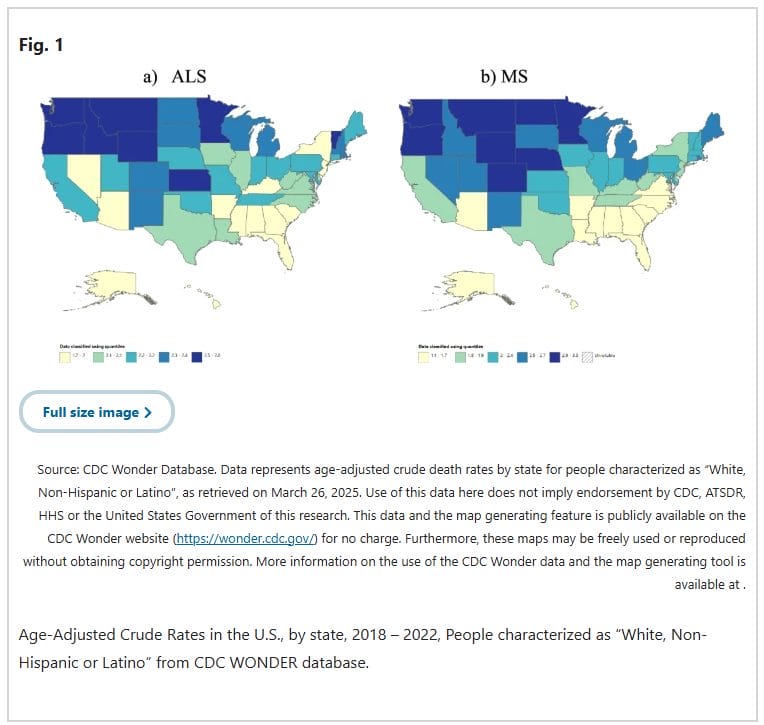
This matters because ALS and MS are typically considered completely different diseases. MS is classified as an autoimmune condition. ALS has not traditionally been. Yet their geographic footprints are nearly identical — and that overlap may be pointing to a shared root cause.
Why This Connection Had Been Missed
Part of the answer lies in a statistical phenomenon called Simpson’s Paradox. When data from men and women were pooled, the correlation between ALS and MS rates disappeared completely. When separated by gender, a very strong relationship emerged — a correlation of 0.75 for women and 0.70 for men, on a scale where 1.0 would be a perfect match.
In other words, the connection had been hiding in plain sight. An artifact of how the data was combined had masked a signal that was there all along. This is a good reminder that absence of evidence is not always evidence of absence — especially in complex diseases like these.
What The Geography Might Be Telling Us
So why do these two diseases cluster together geographically?
The researchers propose several possibilities. One of the most intriguing involves environmental factors that vary by location — including UV light exposure. MS has long been linked to latitude: higher rates occur in northern regions, where sunlight is weaker, and vitamin D levels tend to be lower. Now, that same north-south pattern appears in ALS as well.
Even more striking: once the researchers included each disease in the statistical model for the other, latitude ceased to be a significant predictor of either. This suggests that whatever connects the two diseases to each other may be more powerful than either disease’s individual relationship to latitude — and that light-regulated immune function could be a key piece of the puzzle.
The Role Of Light And Your Immune System
This is where narrowband UVB (NB-UVB) phototherapy enters the picture.
NB-UVB has been used safely for decades to treat autoimmune and inflammatory skin conditions. Research suggests it works by triggering a natural cascade that calms the immune system — reducing the systemic inflammation that underlies conditions like MS, psoriasis, eczema, and more.
For people living with autoimmune fatigue, that chronic inflammation is not just a number on a lab report. It is what makes your body feel depleted, reactive, and unreliable — even on days when nothing seems obviously wrong. Research pointing to light exposure as a regulator of immune function is directly relevant to that experience.
The geographic findings in this study add to a growing body of evidence suggesting that immune regulation — and the environmental factors that influence it, including light — may play a far larger role in neurological and autoimmune disease than previously understood.
What This Means For You
This study does not claim that NB-UVB treats ALS or MS. What it suggests is that systemic inflammation and immune dysregulation may be a shared thread running through multiple neurological diseases — and that environmental factors which regulate the immune system, including light, deserve serious attention.
If you are managing an autoimmune condition, this research is a reminder that you are not imagining the connections you sense between inflammation, environment, and how you feel day to day.
Asking your doctor about additional, non-pharmaceutical approaches to supporting immune regulation is a reasonable and empowered step. The science increasingly supports that conversation.
A Note From Cytokind
If you would like to learn more about how NB-UVB may support your immune health, we invite you to explore our resources at cytokind.net.
- If you have questions about light therapy, you can book a free discovery call with the Cytokind team.
- If you have problems with fatigue, you can take a brief test to determine your Fatigue Severity Score (FSS).
This blog post is for informational purposes only and does not constitute medical advice. Individuals should consult with qualified healthcare providers before beginning any new treatment modality.



